Artificial intelligence has entered Indian healthcare not with spectacle, but with consequence. It now reads scans in district hospitals, flags strokes within minutes, screens diabetic eyes in primary-care clinics and guides surgeons inside operating rooms. For patients, the change is no longer theoretical. It is measurable in time saved, errors avoided and disabilities prevented. India’s experience is increasingly being studied as a case of how to deploy medical AI at scale without surrendering human judgment.
India is among the most demanding test beds for medical AI anywhere in the world. A population exceeding 140 crore, a rapid rise in non-communicable diseases, persistent infectious burdens and chronic shortages of specialists define the landscape. In radiology, neurology, oncology and ophthalmology, demand far outstrips human capacity, especially beyond major cities.
This is precisely where AI has found its role. Not as a substitute for doctors, but as a multiplier of scarce expertise. By compressing decision timelines, prioritising risk and standardising quality, AI allows a limited number of specialists to reach many more patients.
For the common patient, the distinction matters. The doctor is still there. The difference is that the doctor now sees problems earlier and acts faster.
Stroke Care: Minutes Make Difference
Stroke care illustrates AI’s impact with brutal clarity. In India, delayed recognition and referral remain major causes of death and lifelong disability. Every lost minute destroys brain tissue; every delayed scan narrows the chance of recovery.
AI-enabled imaging tools now analyse CT and CT angiography scans within minutes, flagging suspected large-vessel occlusions and alerting teams to the need for urgent transfer. Crucially, the algorithm does not decide treatment, it accelerates certainty. “Artificial intelligence is rapidly becoming an essential ally in stroke care. From faster interpretation of brain imaging to smarter triage in emergency settings, AI is helping clinicians make critical decisions when every minute counts”, says Dr Dheeraj Khurana, in‑Charge, Stroke Program at PGIMER, Chandigarh
Global evidence reinforces this experience. In England, hospitals using AI imaging support in stroke pathways doubled endovascular thrombectomy rates, from 2.3 per cent to 4.6 per cent, by enabling faster identification and transfer, particularly in centres without round-the-clock neuroradiology. The lesson is directly transferable to India: AI matters most where expertise is thinnest.
Radiology: Expert Eyes, Everywhere
Radiology has become the proving ground for AI in Indian healthcare. India’s radiologist-to-population ratio is among the lowest globally, even as imaging volumes continue to rise sharply.
AI systems now triage studies, flag critical findings and prioritise reporting queues. This does not remove the radiologist from the loop; it ensures that attention is directed to the most urgent cases first. “It is a valuable tool that offers vast potential to the healthcare industry at a time of radiologist shortage by using deep learning to capture electronically the expertise of radiologists and clinicians,” says Arjun Kalyanpur, Chief Radiologist & CEO, Teleradiology Solutions, Bangalore, Karnataka
In practice, a CT scan performed in a tier-2 town can now receive expert-level scrutiny within minutes rather than days. Geography, while still relevant, no longer dictates diagnostic quality as rigidly as it once did.
Breast Screening: Evidence Over Excitement
Breast cancer screening demonstrates how AI’s value must be judged not by hype, but by outcomes. Two strong strands of international evidence now converge.
In Denmark, real-world deployment of AI triage reduced double-reading workload by roughly one-third while increasing cancer detection and lowering false positives. In Sweden, the large randomised Mammography Screening with Artificial Intelligence (MASAI) trial involving over 100,000 women showed higher detection rates without increasing recalls, alongside a meaningful reduction in interval cancers, a key indicator of screening effectiveness.
For India, where organised screening remains limited and specialist readers are scarce, these findings matter. Large-scale Indian pilots using AI-based tools have already screened tens of thousands, approaching 100,000 women in some programmes, with peer-reviewed and preprint results pointing to improved early detection. For women, the benefit is direct: earlier diagnosis, fewer unnecessary callbacks and screening systems that work harder without exhausting clinicians.
FathomX’s FxMammo, a National University of Singapore and NUHS spin‑off tool for AI‑assisted mammography, reduces false positives and false negatives while generating heat maps and cancer‑probability scores to speed double reading, and early hospital experience at NUH indicates performance on par with two radiologists, with utility as a triage aid.
In the Indian context, where clinician optimism about AI’s role in earlier detection and workflow relief is high, FxMammo’s “radiologist‑in‑the‑loop” design fits public‑health AI pilots that aim to augment rather than replace expertise and to expand screening capacity across underserved settings.
Diabetes & Eye Care: Blindness is not Inevitable
India’s diabetes burden has turned diabetic retinopathy into a silent epidemic. Vision is often lost not because treatment is unavailable, but because the disease is detected too late.
India’s diabetes burden has turned diabetic retinopathy into a silent epidemic. Vision is often lost not because treatment is unavailable, but because the disease is detected too late.
Validated autonomous/assistive AI systems now screen retinal images in primary care and community settings. Large studies report sensitivities in the mid‑90s, ensuring that patients who need ophthalmic care are identified early. “While many AI systems for diabetic retinopathy are being built, the key issue is validation. Our model was tested on over 3,000-4,000 retinal images. We now have over 95 per cent detection accuracy,” says Dr Rohan Chawla, retina specialist and professor of Ophthalmology, AIIMS New Delhi. For patients with diabetes, this translates into convenience, timely referrals and far fewer missed chances to protect sight.
Inside OT: Hands Still Human
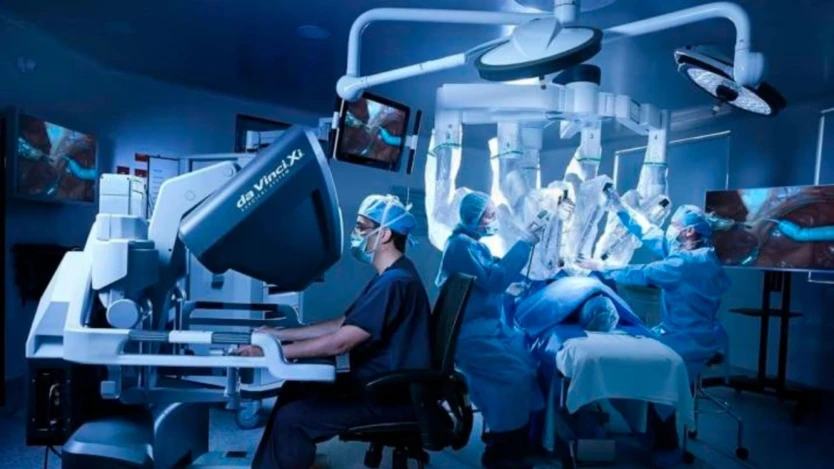
Few areas provoke as much anxiety as AI-assisted surgery. Here, India’s leading institutions have taken a clear stance. Robotics and AI enhance precision, consistency and training, but they do not operate independently.
At AIIMS Delhi, the installation of a dedicated da Vinci robotic training platform alongside advanced simulators signals a strategic choice: build surgeon capability first, then layer technology on top. “Robotic platforms improve precision and recovery, but the surgeon remains central. Technology strengthens skills. It does not substitute them,” says M Srinivas, Director of AIIMS Delhi.
India is not leading the world in inventing medical AI models, but it is emerging as one of the most consequential arenas for deploying them at scale. Market estimates suggest the Indian AI healthcare sector is growing at a compound annual rate of roughly 40.6 per cent, reaching about US$1.6 billion by 2025. Start-ups such as Qure.ai report their tools have already reached over 32 million lives across more than 4,500 healthcare facilities in FY 2024-25 alone.
Clinician sentiment appears aligned with this trajectory. The 2025 Philips Future Health Index for India found that approximately 76 per cent of healthcare professionals are optimistic that AI can improve patient outcomes, with large majorities expecting reduced waiting times and reclaimed clinician hours.
At the policy level, NITI Aayog and national AI roadmaps explicitly position healthcare as a priority sector, backing pilots, capacity-building and responsible AI frameworks across central and state health systems.
Draft guidance issued by the Central Drugs Standard Control Organisation in October 2025 introduces risk-based classification for software as a medical device, lifecycle oversight, and post-market surveillance aligned with India’s Medical Devices Rules 2017. Transparency, bias control and explainability are emphasised, echoing WHO guidance on large multimodal models.
The question is, can AI replace human expertise in medicine? Indian practice answers this daily in clinics, imaging suites and operating rooms. Algorithms can detect patterns and reduce variability. They cannot replace judgment, empathy, accountability or ethical reasoning. “With high tech, we should not lose the high touch, as no instrument, no technology, no equipment can replace the human touch and the compassion towards the patient,” says Dr Srinivas.
India is not choosing between doctors and machines. It is building a system in which clinicians lead and AI assists, scaling expertise without surrendering humanity. If this balance holds, India’s model may offer the world one of its most important lessons yet: the future of medicine belongs not to artificial intelligence alone, but to intelligent clinicians who know how to command it.
For patients, AI is not about machines taking over medicine. It is about fewer missed diagnoses, faster treatment, safer surgery and fairer access, whether one lives in a metropolitan centre or a small town. The impact is becoming tangible across the country.
(Dr Anish Desai is a healthcare entrepreneur. He is leading IntelliMed Healthcare Solutions)